ARGUMENTS TO MAKE TO SHOW MASK SCIENCE FICTION - PART 3
Masks and N95s were never the proper tool for the job.
My apologies for the time away from these articles but I want to continue the “Arguments to Make” series on why masking is pure science fiction. In the previous article I discussed the aspects of the viral particle and in this I want to expand on that and include more information as to why the masks and N95 respirators are not the tools for the job.
I have used an RCT from Brazil as guidance for N95 respirator deployment in the workplace. It is important to know that most surgical masks and N95s will degrade after 4 hours of use in a medical setting but its degradation in work environments without the superior indoor air quality features found in a medical work environment. The more heat and moisture a face covering is exposed the faster the degradation. Especially harmful to the mask is the wearer’s heat and moisture which comes from the wearer’s breath and perspiration.
It is critical in examining masks to differentiate the abilities of respirators and masks. Then match the proper tool to the task. This clearly shows that the N95 respirator and surgical mask is no match for environments without proper indoor air quality.
If you can see visible dust in around you, that dust is on the level of about 50 microns. The virus is 500 times smaller than that dust you can see. If you look at a cross section of a human hair, the COVID particle is around 1,000 times smaller than that human hair cross section. This simple fact demonstrates that the particle can easily escape through a mask. It’s a super-freeway for the virus to come and go, and I prefer to call is “source redirect”...my fun counter to the “source control” claim.
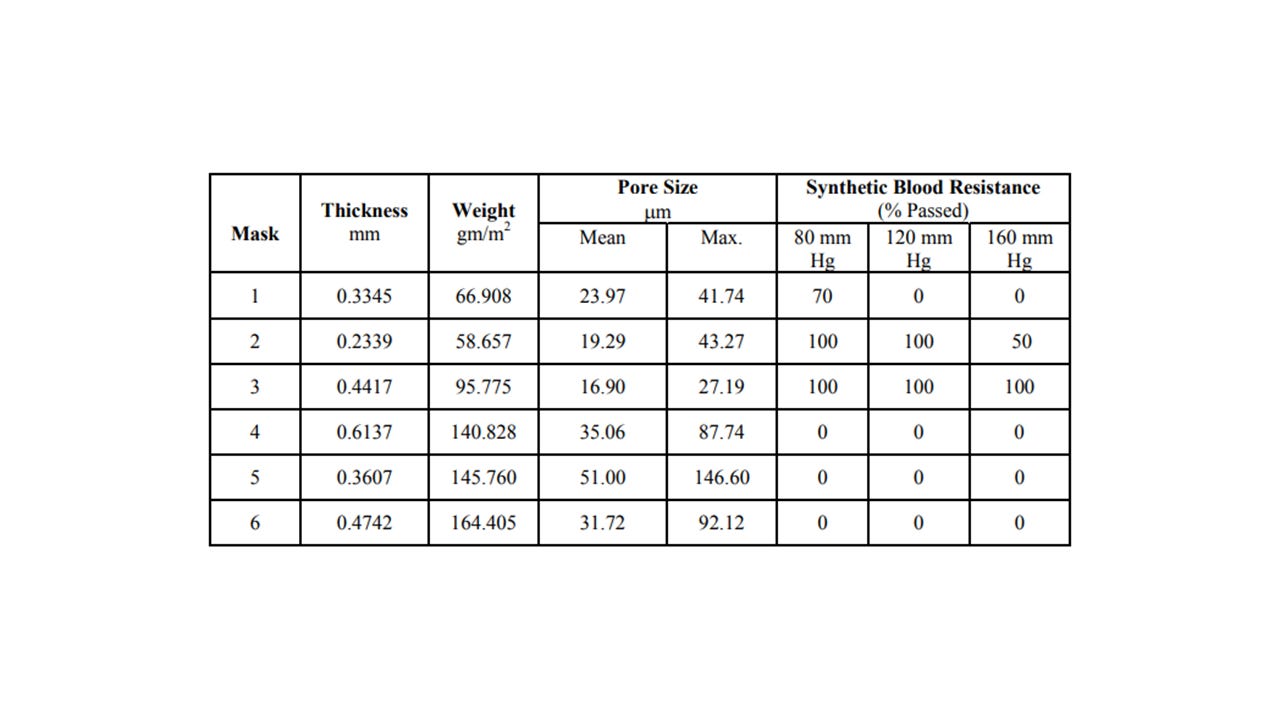
This is fact of the mask not having the proper mechanics for the job is further illustrated in a 2003 study from North Carolina State University, that reviewed the pore size of the most used masks in the medical field. The study demonstrates that the front mask pore size is at minimum 16.9 to 51 microns in size, which means viral particles can pass through. This further illustrates that the source control argument is bogus.
References:
o “Influence of wearing time on efficacy of disposable surgical masks as microbial barrier”; Publication in the Brazilian Journal of Microbiology; Authors: Maria Helena BarbosaI, Kazuko Uchikawa Graziano.
o “The Relationship of Fabric Properties and Bacterial Filtration Efficiency for Selected Surgical Face Masks”; NC State University; Authors: Karen K. Leonas, Ph.D., Cindy R. Jones.
o ASTM Standard F3502 - 21: Standard Specification for Barrier Face Coverings.
o “Aerosol filtration efficiency of household materials for homemade face masks: Influence of material properties, particle size, particle electrical charge, face velocity, and leaks”; Authors: Frank Drewnick, Julia Pikmann, Friederike Fachinger, Lasse Moormann, Fiona Sprang & Stephan Borrmann.
o “Exhaled aerosol increases with COVID-19 infection, age, and obesity”; David A. Edwardsa, Dennis Ausielloc, Jonathan Salzmanb, Tom Devlinb, Robert Langerd, Brandon J. Beddingfielde, Alyssa C. Fearse, Lara A. Doyle-Meyerse, Rachel K. Redmanne, Stephanie Z. Killeene, Nicholas J. Manesse, and Chad J. Roy.